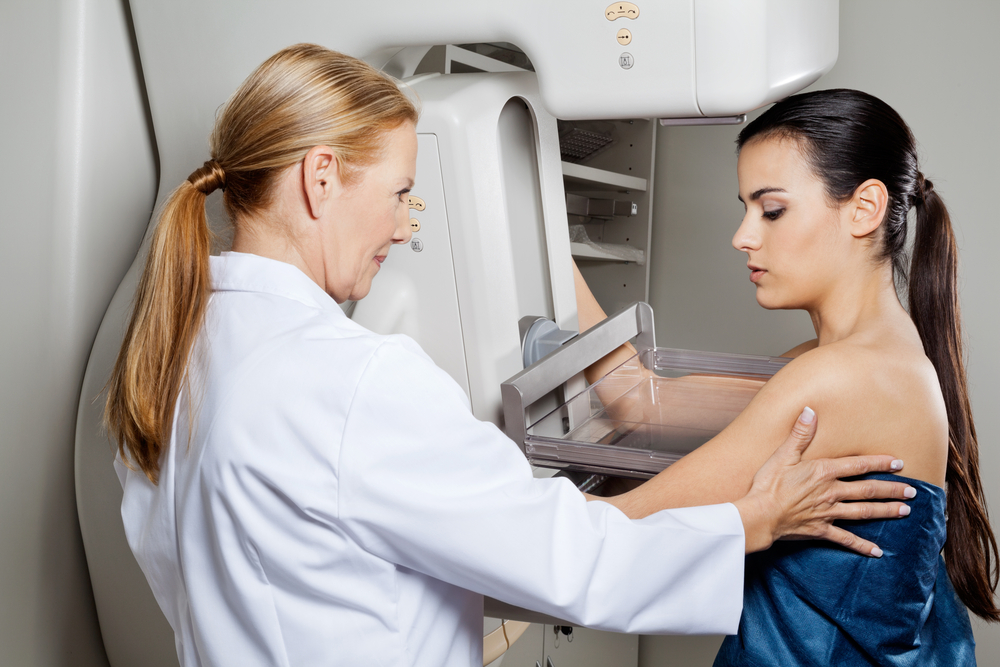
 A study from the University of California, San Francisco (UCSF) revealed screening mammography that relied mostly on risk-based triage (strong family history, dense breast tissue, etc.) missed a significant number of cases of invasive breast cancer, especially among women aged 40 to 49 years old.
A study from the University of California, San Francisco (UCSF) revealed screening mammography that relied mostly on risk-based triage (strong family history, dense breast tissue, etc.) missed a significant number of cases of invasive breast cancer, especially among women aged 40 to 49 years old.
The study was led by Dr. Bonnie N. Joe, M.D., Ph.D., an associate professor in residence and chief of women’s imaging at UCSF, and presented during the Radiological Society of North America (RSNA).
Dr. Joe explained that breast cancer screening for women between 40 and 49 years of age continues to be a subject of debate among experts. Several recent studies recommend risk-based screening based on family history and breast tissue density, but Dr. Joe and her co-investigators found this approach was not reliable enough, and would give rise to missed invasive breast cancer diagnoses.
The UCSF study enrolled 136 women in a similar age bracket, diagnosed with breast cancer from screening mammography between the years 1997 and 2012. Patients with active symptoms, and those who had a personal history of breast cancer were excluded from the research. Researchers then gathered patient data on family history, breast density, type of malignancy, lymph node status, and tumor receptor status. “We found that almost 90 percent of the invasive cancers we would have missed using risk-based triage had positive receptor status, meaning they were very treatable and worth finding early,” Dr. Joe said in a press release.
Out of the 136 breast cancer patients, 50% were found to have an invasive form, while the other 50% had ductal carcinoma in situ (DCIS). Out of the latter half, 88% were intermediate or high grade. The researchers noted 90% did not have a strong family history of breast cancer, and 86% did not have dense breast tissue. In total, 78% percent had neither of the two risk factors, including nearly 80% of those diagnosed with invasive breast cancer.
[adrotate group=”3″]
Dr. Joe explained that using a risk-based approach would negate the very purpose of screening mammography, which is to catch the disease in the earliest stage possible to improve survival. This highlights the need to reevaluate the triage criteria for breast cancer screening as family history and tissue density may not be enough.
While the American Cancer Society and American Medical Association generally recommend yearly screening mammography beginning at age 40, the United States Preventive Services Task Force released a contradictory set of guidelines suggesting screening mammography be done biannually, starting at age 50. Based on the findings of this study, Dr. Joe still recommends the ACS and AMA guidelines be followed to maximize the benefits of screening mammography.