 This is the second guest column by Rachel Andrews of Gloucestershire, U.K., a Breast Cancer News reader who developed severe lymphedema as a result of her cancer and underwent a microsurgery procedure intended to correct that condition. Rachel described the procedure, called LVA, in her May column and now returns for a one-month update, informing readers about the procedure and how recovery is going for her.
This is the second guest column by Rachel Andrews of Gloucestershire, U.K., a Breast Cancer News reader who developed severe lymphedema as a result of her cancer and underwent a microsurgery procedure intended to correct that condition. Rachel described the procedure, called LVA, in her May column and now returns for a one-month update, informing readers about the procedure and how recovery is going for her.
On May 30, I chose to have LVA (lymphatico-venular anastomosis) surgery in an attempt to treat the lymphedema that developed in my left hand and arm as a result of breast cancer. Here is an update on how the surgery went for me, and my hopes for how recovery will continue to go.
The procedure was to be undertaken using local anesthetic, so I was able to have my breakfast. I walked to the anesthetic room and was greeted by two surgeons. The plan was for the two surgeons to work alongside each other throughout the surgery. It was anticipated to last between four and six hours, so I was offered a urinary catheter, which I declined!
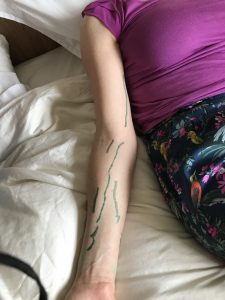
Prior to commencing the surgery, the lymphography procedure was repeated on both my affected and unaffected arms. This involves two local anesthetic injections in the wrists and injection of dye under the skin. The lymphatic flow on both of my arms was marked with a marker pen. This was unclear in the affected arm, so the location of lymph channels was mirrored from my good arm to give the surgeons an indication of where to make the incisions.
The nursing staff helped me into position on the operating table, and my left arm was prepared for surgery and then placed outstretched, with my palm facing upward on a sterile field. The surgeons positioned themselves either side of the table on which my arm was placed, and each used microscopic surgery equipment. There was a screen on which I could watch, and duly did, once the initial incision had been made.
So it began! Five hours, two surgeons, and four incisions. I was required to lie still for the entire duration of the surgery with the exception of a very brief break in the middle, just enough time for me to wriggle a little and for the surgeon to change the music! I had requested some Kate Rusby, as I find her music calming, but unbeknownst to me, the music couldn’t be changed until this break — after a full two-and-a-half hours, I feel that I like her a little less!
As the surgery was performed under local anesthetic, repeated fine injections were necessary, but the discomfort was minimal and the local acted well throughout. My only discomfort was lying with my shoulder rotated out for a couple of hours, and I requested some paracetamol to ease this.
Each incision was different, as the anatomy found differed in each location. I have one incision just above my wrist, two on my forearm, and one on the inside of my upper arm. The surgeon’s goal was to stitch lymph channels into veins, and this required a painstaking search for these tiny vessels. One incision has five lymph vessels attached to one vein, another brought two into one vein, and then two incisions where there were two connections were made using two veins and two lymph channels.
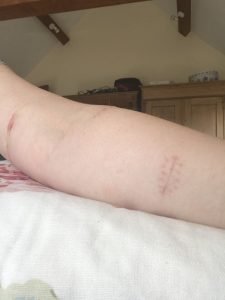
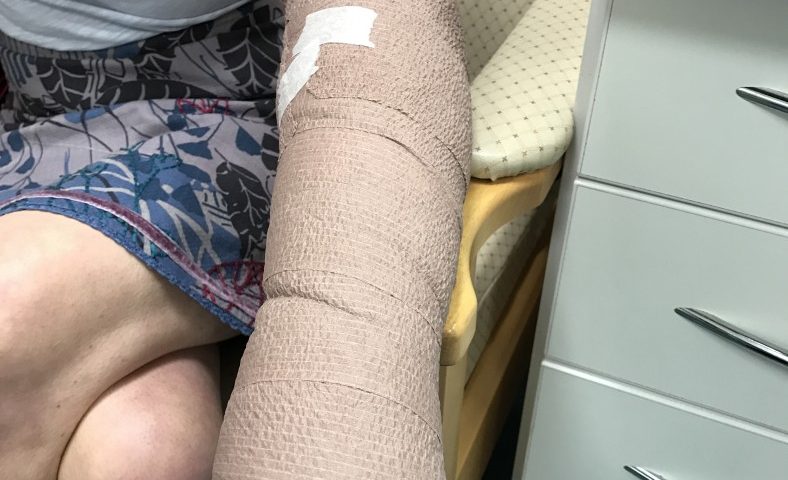
The surgery lasted five hours, and I was able to chat to the surgeons throughout. Once I was stitched up, I had dressings applied and was then able to sit up. I returned to the day room and had lunch. I was given antibiotics to take, as infection is the biggest risk, and returned home that afternoon.
The surgeons request that no compression be applied to the limb for a week after surgery, and no significant improvement is anticipated for up to three months. It is expected that things will continue to improve gradually for up to a year post-surgery. Despite this, I saw an immediate improvement in my hand, and after 12 hours, the arm became softer and less turgid.
I am now nearly four weeks post-surgery and am elevating my arm and massaging it at every given opportunity — although my twin sons celebrated their 21st birthdays this weekend, so I am not resting as much as I’d like! I am really hopeful that there is progress being made and my comfort levels are improving. I have not needed to take any pain relief with the exception of two paracetamol the following morning. This is not a painful procedure as the incisions are not deep.
I will update readers after the three-month period, following my review by the Oxford Lymphoedema Practice. Fingers crossed that all will continue to improve. I am so grateful that I have had the opportunity to have this surgery, as things would have gotten progressively worse for me. I hope this prompts others to possibly consider it for themselves.
***
Note: Breast Cancer News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Breast Cancer News, or its parent company, BioNews Services, and are intended to spark discussion about issues pertaining to breast cancer.

That is fantastic, so happy for you! I am considering the same procedure. I had a lymph node transfer with a DIEP reconstruction and before I went home I had noticed a change in my arm. The surgeon was unsure if it would do anything at all. I noticed an immediate change, then had my arm measured, the change was 2.5cm in the upper arm. The forearm has improvement of about 1cm. I have since had my arm mapped (3 months post surgery), and it confirms a superhighway to a node in my armpit which is the transplanted node. The lower arm is struggling though, so I am considering additional surgery as it would be lifechanging. I am surprised that it didn’t require an anaesthetic. Was it expensive? Best wishes for continued improvement x
hello
I read about LVA lymphodemia treatment. had masectomy 3 yrs ago , about 2 yrs later, developed Lympho in arm/hand. I have not heard about this LVA treatment. can anyone advise approx cost of this – is it only carried out at a Oxfordshire, hospital ? can the consultant tell you if this treatment is advisable before you proceed ? presumbly, this is not carried out under NHS treatment. I wish I’d been given more info re Lympho – never heard of it until I got it !!!
sorry – so many questions. be grateful for help.
Following. Thanks for keeping us updated! Best wishes from another lympheDiva ?
As an Occupational Therapist Who not only treats lymphedema, but is going through breast cancer myself, I find this news to be very exciting and uplifting! Please keep us posted on your progress !!!
We are sorry to hear about your diagnosis with breast cancer, but are glad that you found some encouragement through our post. We will definitely be keeping people updated as the newest research becomes available.
Hello, I have booked a consultation to see if I’m suitable for LVA, I feel if I am then I will need to have a general anesthetic as I am such a mardy. I’m worried about the procedure, but also excited if it will work, its my leg that is swollen after only 1 lymph node removed (sentinel) its only 1 inche bigger than my other leg from the knee down and in places only 1/2 inch, but I love to do amateur dramatics and also feel it may get worse as I get older, plus I don’t like wearing the support stocking in the summer, although I put it on as soon as I wake until I go to bed, any feed back would be appreciated many thanks
Hello Julie, i am writing to ask if you went ahead with the LVA procedure on your leg? I have lymphoedema in my left leg and it’s about an inch bigger all over. Like you i hate wearing the stocking and do think it’ll get worse as i get older (I’m 47), so i am looking at funding the LVA operation. I’ve had it for about 2 years (since my cancer surgery). I’d really appreciate some feedback if you can help?
This is fantastic. Please update us on your progress. I had this surgery under anesthesia (7.5 hours) in February. Dye was injected between my knuckles but diffused at my wrist, so they only did connections in my hand. I am very impressed that your surgeons went in and found the vessels for connection without the mapping. Unfortunately, my situation has not improved and I’m researching next steps.