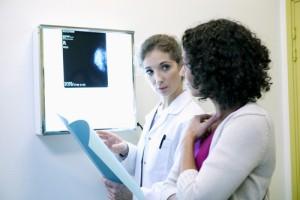
 Of the 4% of breast cancer patients with inflammatory breast cancer, 33% are not treated appropriately, putting them at risk for poor prognoses. For some patients, receiving the proper care regimen can be influenced by their choice of care provider.
Of the 4% of breast cancer patients with inflammatory breast cancer, 33% are not treated appropriately, putting them at risk for poor prognoses. For some patients, receiving the proper care regimen can be influenced by their choice of care provider.
“I feel like the decision saved my life,” said Lourdes Suggs, a woman with inflammatory breast cancer, who was treated at MD Anderson’s Morgan Welch Inflammatory Breast Cancer Program following her diagnosis with breast cancer. “I’m cancer-free now, and I’m looking forward to a long future with my grandchildren. I don’t think I’d have five years if I’d stayed in Georgia for treatment,” she said to reporter Todd Ackerman in an article on the Houston Chronicle.
MD Anderson began its pioneering program in 2006 as an effort to provide expert care to as many patients with inflammatory breast cancer as possible. The center is devoted to its patients, which number approximately 100 annually, and strives to mitigate the 45 – 60% five-year mortality rate for inflammatory breast cancer.
A group of researchers at MD Anderson, which included executive director Dr. Naoto Ueno, was interested in the number of patients who do not receive the standard of care for inflammatory breast cancer. They published their findings in Journal of Clinical Oncology. “Underuse of Trimodality Treatment Affects Survival for Patients With Inflammatory Breast Cancer: An Analysis  of Treatment and Survival Trends From the National Cancer Database“ was written with the goal of identifying a relationship between survival and treatment regimen for patients with inflammatory breast cancer. The team had a notion that a large number of inflammatory breast cancer patients are not properly treated.
of Treatment and Survival Trends From the National Cancer Database“ was written with the goal of identifying a relationship between survival and treatment regimen for patients with inflammatory breast cancer. The team had a notion that a large number of inflammatory breast cancer patients are not properly treated.
Delving into the National Cancer Database, an oncology outcomes database for more than 1,500 hospitals, the team found records for more than 10,000 women treated for non-metastatic inflammatory breast cancer between 1998 and 2010. Of these women, 58.4 – 73.4% were treated with chemotherapy, mastectomy, and radiation, the standard recommended treatment to be given in the order listed. A peak occurred in 2004 (at 73.4%) and was followed by a study decline to 65.9% in 2010.
“These numbers are kind of shocking,” said Dr. Ueno. “The treatment’s a no-brainer. It’s standard care, nothing new.” Overall, 55% of triple treatment patients were alive after five years, outnumbering the 43% who received only surgery and chemotherapy and 41% who received only surgery and radiation.
Treatment is not such a no-brainer if doctors miss the diagnosis of inflammatory breast cancer. “If [patients] go to places without the specialized expertise, they’re risking their lives,” said Dr. Ueno. Inflammatory breast cancer is characterized by red inflammation in the breast and microscopic tumor cells in lymph vessels. In Suggs’ case, symptoms included an enlarged, warm breast with a suddenly orange peel texture. These symptoms and follow-up tests can be missed if a cancer center does not have a dedicated pathologist with inflammatory breast cancer expertise, according to Dr. Massimo Cristofanilli, director of the breast care center at Sidney Kimmel Cancer Center in Thomas Jefferson University and previous director of the program at MD Anderson.
“In the community there’s a lack of understanding about the complexity and aggressive nature of inflammatory breast cancer,” explained Dr. Cristofanilli. “It’s frequently treated not in a multidisciplinary fashion but using a sequence of modalities based on local availability.” By increasing clinician awareness about the signs of inflammatory breast cancer, patient survival may improve and the number of patients with “weird” treatment histories may decrease.

