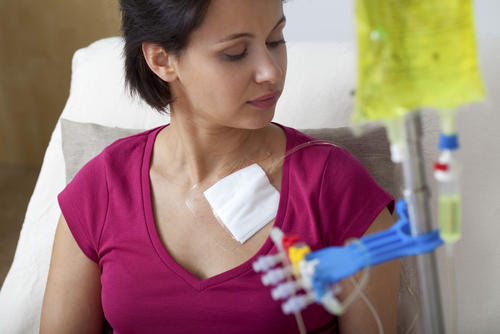
 A new hope for women with breast cancer is being pursued through the development of neoadjuvant chemotherapy.
A new hope for women with breast cancer is being pursued through the development of neoadjuvant chemotherapy.
Neoadjuvant therapy is a treatment given to patients before their primary treatment, usually either a mastectomy (removal of one or both breasts) or a lumpectomy (tumor and a small amount of tissue around it is removed).
Now, results from a clinical trial involving approximately 12,000 women, presented at the 2014 Breast Cancer Symposium entitled, “Locoregional recurrence (LRR) after neoadjuvant chemotherapy (NAC): Pooled-analysis results from the collaborative trials in neoadjuvant breast cancer (CTNeoBC),” prompted researchers to hypothesize that women with breast cancer who respond favorably to neoadjuvant chemotherapy might be spared radiotherapy and even be subject to far less extensive surgery.
The study’s lead investigator Eleftherios Mamounas, MD, MPH noted growing agreement among researchers and clinicians in breast cancer treatment: to choose breast cancer patients who have optimal conditions to go without treatment after surgery. Therefore, identifying independent predictors of recurrence is of the utmost importance.
The findings showed that pathologic complete response (pCR) and tumor subtype are “strong predictors” of cancer recurrence, local and regional, in breast cancer patients with neoadjuvant chemotherapy.
Many studies indicate similar effects of adjuvant and neoadjuvant chemotherapy on the outcomes of breast cancer. Hence, information specific of the latter, such as pCR, allows clinicians to identify patients who can skip radiation. Moreover, patients who fully respond to neoadjuvant chemotherapy might decrease mastectomy and lymph node removal.
As part of the study, Dr. Mamounas and colleagues reviewed 12 clinical trials of neoadjuvant chemotherapy. These studies were performed in women with breast cancer (stage, I to III) and included 11,955 patients with pCR data and a median follow-up of 5.4 years.
[adrotate group=”3″]
The researchers used clinic-pathologic factors, such as pCR and breast cancer subtype, to identify and assess independent predictors of locoregional recurrence (LRR). Although LLR 5-year rate was “low” (8.3%), the rates varied with tumor subtype, said Dr. Mamounas.
Age was an independent predictor of LRR only in patients who had undergone lumpectomy. On the contrary, pCR in the breast and pathologic axillary nodal status were independent predictors of LRR on patients with both conditions, mastectomy and lumpectomy.
Despite being the largest study on this research topic, additional data is necessary to support future guidelines and before changes to the current practice can be recommended, cautioned Dr. Mamounas.